Some dementia and general health clinics now advertise a groundbreaking new treatment for dementia: hyperbaric oxygen therapy (HBOT). While this treatment does have some potential, most clinics oversell the positive effects HBOT has on patients with dementia. In reality, research is very much still ongoing. Many of the studies published only involved a small number of participants and did not examine the long-term effects.
Since we do not yet offer hyperbaric oxygen therapy at our dementia clinic (but are waiting for more research to come out before making the decision), we believe we can give you an unbiased opinion. In this article, we explore if and how HBOT is beneficial for patients with dementia.
We then go on to cover alternative dementia treatments, including therapy sessions at our clinic, Neural Effects. These include a combination of exercise and cognitive stimulation therapy to slow down cognitive decline and help patients maximize their independence.
Neural Effects uses the latest evidence-based techniques to diagnose and help patients of dementia. We are located in Provo, Utah and serve anyone in the Salt Lake City or the Utah County area. We are in network for most types of medical insurance. Schedule your evaluation today.
Is Hyperbaric Oxygen Therapy (HBOT) Beneficial for Patients with Dementia?

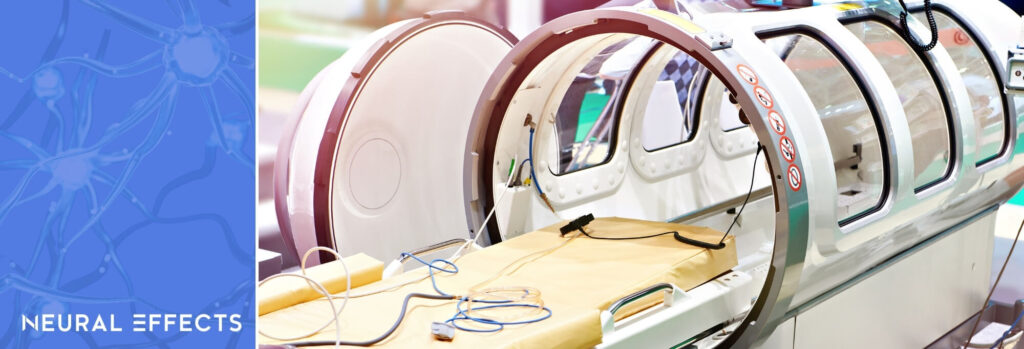
During hyperbaric oxygen therapy (HBOT), patients breathe pure oxygen inside a special pressurized chamber. (Pressure in the chambers is 1.5–3 times higher than atmospheric pressure.) HBOT is a well-established treatment for decompression sickness (a complication that can arise while scuba diving), but it can also be used to treat some other conditions, including carbon monoxide poisoning, radiation injury, wounds that are difficult to heal, and severe traumatic brain injury.
Given positive results with stroke patients, several research groups around the world started to wonder whether HBOT could also be beneficial for patients with dementia. The idea is that flooding the patient’s brain with oxygen may improve cognitive function and alleviate symptoms such as memory loss, poor attention, and so forth.
In 2009, one of the first studies showed that HBOT improved cognitive function in patients with vascular dementia when combined with donepezil. A later study followed a 58-year-old dementia patient who, after multiple sessions, reported increased levels of energy, better mood, and improved cognitive and language function, as well as reduced anxiety and frustration.
More recent studies looking at the impact of hyperbaric oxygen treatment showed that this technique can improve blood flow and reduce the level of amyloid plaques in the brain. (A notable amyloid burden is one of the hallmarks of Alzheimer’s disease.) The authors suggested that HBOT triggers the production of stem cells, which in turn promotes the formation of new blood vessels and increases cerebral blood flow (blood flow in the brain). Ultimately, this reduces brain hypoxia (low oxygen) and improves cognitive performance.
Over the past few years, a growing number of studies have added further speculation as to how HBOT might help elderly patients’ brain function and overall health:
- Increase oxygen supply and tissue oxygen partial pressure (pO2)
- Relieve cerebral edema
- Decrease intracranial pressure
- Promote brain tissue healing
- Improve metabolism
- Reduce cell death (apoptosis)
- Alleviate oxidative stress
- Increase mitochondrial function
- Trigger production of stem cells
- Promote cell differentiation and regeneration
- Increase access to oxygen for damaged tissue
- Promote new blood vessel formation (angiogenesis)
- Improve glucose metabolism in areas associated with executive function, language, and memory
Nevertheless, most of these benefits are still just a possibility. More research and clinical trials are needed.
All that said, increasing oxygen levels (O2) in the brain isn’t always beneficial. Brain cells cannot use this extra oxygen arriving in the bloodstream if there isn’t enough carbon dioxide (CO2) around. With low CO2 levels, O2 remains bound to hemoglobin and is not released into the cells. In contrast, high levels of CO2 lower the affinity of O2 to hemoglobin, allowing this gas to be used by cells. This is called the Bohr effect, and it represents the body’s way to deliver oxygen where it’s most needed. (Increased CO2 production means an active metabolism.)
This means any benefits of HBOT are likely to be short-lived because the concentration of CO2 needs to stay high enough relative to oxygen concentration. For example, one study found that any improvements in cognitive abilities after a few HBOT sessions were still visible after one month but not after three or six months. This suggests that HBOT may temporarily ameliorate cognitive impairment in patients with neurodegeneration, but the effect is not permanent.
It’s easy to suggest that if patients just keep attending HBOT sessions, it may prolong the therapeutic effects. Unfortunately, long-term use of HBOT can lead to unpleasant side effects. Even if patients experience benefits during the initial sessions, in the long term, they may start to experience confusion, problems with balance, aches and pains, and even cataracts as a side effect of HBOT. If you’re receiving HBOT treatments and begin to develop these symptoms, consult with your doctor and consider stopping HBOT.
Overall, our advice is to be cautious about HBOT sessions for patients with dementia. If you want to try it, discuss it with your doctor first and track your improvements to determine if it’s helping you or not. Below, we’ll give you a few ways to track your progress.
Ways to Track Your Improvements After HBOT Sessions

There are many ways to track your symptoms, and not all of them will suit every patient. Here are two options to monitor the effect of hyperbaric oxygen therapy on your wellbeing:
- Write a daily journal: One good routine for patients with dementia is to keep a daily journal. A daily journal can help the patient track their symptoms and express their feelings in writing. Any method will do — from using a pen and paper to downloading an app on your phone. Use whatever you can do the most consistently. These notes are ideal to share with doctors and caregivers.
- Monitor physical health indicators: Patients can also use wearable devices to measure a variety of body functions, including sleep quality, physical activity, stress, blood pressure, and heart rate variability. For example, sleep disturbances are common in dementia, but using a device such as a Whoop bracelet or an Oura ring allows patients to detect changes and see a doctor if needed.
Alternative Treatment Options
Hyperbaric oxygen therapy is a novel approach to treat dementia patients. The technique is showing some promising results, but it is still undergoing scrutiny by the scientific community to determine if it is a worthwhile treatment for patients with dementia.
In the meantime, there are some alternatives that you may want to consider:
- Treatment at Neural Effects
- Lifestyle changes
Treatment at Neural Effects

Treatment for dementia at Neural Effects involves a combination of cognitive stimulation therapy (CST) and exercise to delay cognitive decline and improve the patient’s quality of life. Exercise is a crucial part of the treatment. It triggers the release of important chemicals in the brain, which help the patient become more receptive to therapy. One of these chemicals is called brain-derived neurotrophic factor (BDNF), which stimulates memory and learning.
Before treatment starts, our patients complete a neuropsychological exam (also called a neurocognitive evaluation). This exam takes about 2–2.5 hours to complete. Our therapists assess cognitive skills (such as attention and memory), physical abilities (such as reflexes and balance), and emotional symptoms (such as anxiety and depression).
All this information is then combined to create a cognitive care plan (CCP). Every patient we assess receives their CCP, even if they decide not to continue treatment at our clinic. The report contains useful information that patients and their caregivers can use to improve their quality of life. The CCP includes:
- Results from the assessment
- Risk factor analysis and thoughts on likely disease progression
- Lifestyle changes that may help the patient
- Ways the family can get involved
- Recommended treatment options
Patients with mild cognitive impairment or who are in the early stages of dementia who wish to get treatment at Neural Effects can do individual therapy sessions or start a course of fourteen group therapy sessions. Typically, sessions run twice a week for seven weeks. Sessions start with a few minutes of aerobic exercise, usually done on a treadmill or stationary bike. Our therapists are trained to accommodate patients’ mobility issues or other health conditions.
After exercise, patients start their CST part of the session. This includes a variety of activities to help cognitive skills, such as discussing current affairs, playing board games, listening to music, or doing arts and crafts. If our therapists feel that patients may benefit from additional therapy or medical treatment, we refer them as needed to the appropriate specialists.
For our first CST session, we invite family members and caregivers to attend to learn more about our treatment. This way, they can support patients at home by repeating some of the activities and games. Our therapists also give family members additional information regarding local resources and lifestyle changes (see below) that can help loved ones improve their quality of life.
Neural Effects uses the latest evidence-based techniques to diagnose and help patients with dementia. We are located in Provo, Utah and serve anyone in the Salt Lake City or the Utah County area. We are in network for most types of medical insurance. Schedule your evaluation today.
Lifestyle Changes

Lifestyle changes are one of the best ways to help slow down the progression of dementia symptoms. These include:
- Challenging the brain: Patients with dementia should keep their brains active with cognitive activities, such as playing games and puzzles, learning a new skill, or engaging in activities that require coordination, such as arts and crafts. Our recommendation is to engage in these activities for at least 30 minutes every day. Pick something you enjoy doing and can still complete without getting frustrated.
- Engaging in regular exercise: Regular physical activity improves fitness and promotes better cardiovascular health. It also slows cognitive decline, improves mood, and promotes better sleep. Any type of activity can help, especially if it increases heart rate. Examples include walking, dancing, or gardening. Ideally, patients should engage in 30 minutes of exercise per day, five to seven days per week.
- Participating in social activities: The best way to reduce the risk of anxiety and depression is to stay socially active. Consider going out with friends, joining a new group, or taking dance lessons. Patients can also look for support groups in their area, both for the patient and caregivers.
- Eating a balanced diet: Following a healthy diet is another form of slowing down cognitive decline. One example is the MIND diet, which includes green leafy vegetables, berries, nuts, whole grains, fish, and poultry, while minimizing red meat, dairy products, sweets, and fried food. Patients can also choose to follow the Mediterranean diet or the Dietary Approaches to Stop Hypertension (DASH) diet. Both encourage eating plenty of fruits and vegetables and avoiding sugary treats and processed food. At our clinic, we primarily teach the Mediterranean diet.
- Follow a healthy sleep pattern: Sleep disturbances are common with dementia. This may include difficulty falling asleep at night or drowsiness during the day. Some dementia patients also experience “sundowning,” where they feel confused, agitated, and aggressive in the evening. Patients are advised to follow strict bedtime routines by going to bed and getting up at the same time every day. Also, patients should avoid caffeinated drinks, limit the use of screens before bed, and end the day with a relaxing activity, such as listening to music or reading a book. If patients are still struggling, they may want to try melatonin, a supplement that helps improve sleep and reduce sundowning. You can start with a low dose (2 mg slow-release is common) 30 minutes before bed and increase on the advice of a specialist.
Neural Effects uses the latest evidence-based techniques to diagnose and help people with dementia. We are located in Provo, Utah and serve anyone in the Salt Lake City or the Utah County area. We are in network for most types of medical insurance. Schedule your evaluation today.