Receiving a dementia diagnosis is not easy for any patient, but for those younger than 65 years of age, the diagnosis is even harder to accept. Processing your emotions takes time, and there’s much to plan for your future. Getting a treatment plan together is an important priority once you get your diagnosis, but it’s not always as simple as it should be.
Often, even healthcare professionals working in dementia care are inexperienced in addressing the special needs of this younger group of patients. Virtually all dementia services and interventions are geared toward people aged 65 years and over. Many patients and their families struggle due to inadequate support.
At Neural Effects, we can diagnose and treat early-onset dementia. In fact, our treatment approach — a combination of aerobic exercise and cognitive stimulation therapy — is most effective for mild cognitive impairment (MCI) and the early stages of dementia. Our program is well-suited to help patients of all ages with a medical history of dementia symptoms.
In this article, we’ll answer the following questions:
- What is early-onset dementia?
- What types of dementia can affect younger patients?
- What are the best treatment options for early-onset dementia?
- How can you plan around early-onset dementia?
- What are some additional steps you can take at home to delay the progression of dementia symptoms?
Neural Effects uses the latest evidence-based techniques to diagnose and help dementia patients. We are located in Provo, Utah and serve anyone in Salt Lake City or the Utah Valley area. We are in network for most types of medical insurance. Schedule your evaluation today.
What Is Early-Onset Dementia?
Dementia is a neurodegenerative disease that causes a progressive decline in a person’s ability to think, reason, communicate, and remember. Personality, behavior, and mental health are also affected.
If the patient is younger than 65 years old at the time of diagnosis, it’s considered young-onset or early-onset dementia. Patients can be diagnosed in their 30s, although this is extremely rare. Most commonly, early-onset dementia patients are between 45 and 65 years old when they’re diagnosed. This is not a common condition, but it affects around 80 to 140 patients out of every 100,000 individuals. There is no biological reason for this division; it’s simply based on the fact that 65 was the usual retirement age for many people.
When compared to older patients with dementia, younger patients are more likely to:
- Have a rarer form of dementia, such as atypical Alzheimer’s disease.
- Experience symptoms affecting behavior, social functioning, balance, and coordination.
- Have an inherited form of dementia.
- Experience stronger psychological and physical distress.
- Experience employment issues.
- Experience financial issues.
- Have a younger and more dependent family.
- Have additional responsibilities caring for parents.
Since family history is one of the only known risk factors for early-onset dementia, and dementia is frequently considered a condition associated with old age, symptoms of early dementia onset are not always recognized as such. They might be attributed to stress, depression, or menopause, which often leads to significant delays in getting a diagnosis.
However, an accurate and early diagnosis is crucial. It allows patients to start treatment as early as possible and plan for their future. It also helps to rule out other potential causes for symptoms, such as depression or nutritional deficiencies.
Further reading about conditions commonly mistaken for dementia can be found in this post: Can dementia be reversed?
What Types of Dementia Can Affect Younger Patients?

Patients with early-onset dementia can be diagnosed with any type of dementia — Alzheimer’s, frontotemporal dementia, Lewy Body dementia, Parkinson’s disease, and so forth. But young patients often experience different symptoms compared to older patients with the same type of dementia.
Alzheimer’s Disease
Alzheimer’s disease is the most common form of dementia in young patients, affecting 1 in 3 early-onset dementia patients. That’s still less frequent than in older populations, where 2 out of 3 dementia patients are diagnosed with Alzheimer’s disease.
Some researchers hold that early-onset Alzheimer’s disease is not the same condition as that found in older patients. Often, memory loss is not the first change that patients notice. Instead, patients may find they are sleeping more, becoming aggressive and short-tempered, or are disinterested in things around them. In addition, some studies show that younger patients often have a higher burden of amyloid plaques and lose cognitive skills faster when compared to older individuals.
People with Down Syndrome have a high risk of developing early-onset Alzheimer’s. Although the reasons are not fully understood, it’s believed that the extra copy of chromosome 21 leads to an excessive amount of a precursor of amyloid protein, which in turn can form plaques in the brain characteristic of Alzheimer’s. By age 40, many patients with Down’s syndrome have changes in the frontal lobe of their brain caused by these plaques, and by age 65, more than 80% of these patients develop symptoms of dementia.
Atypical Alzheimer’s Disease
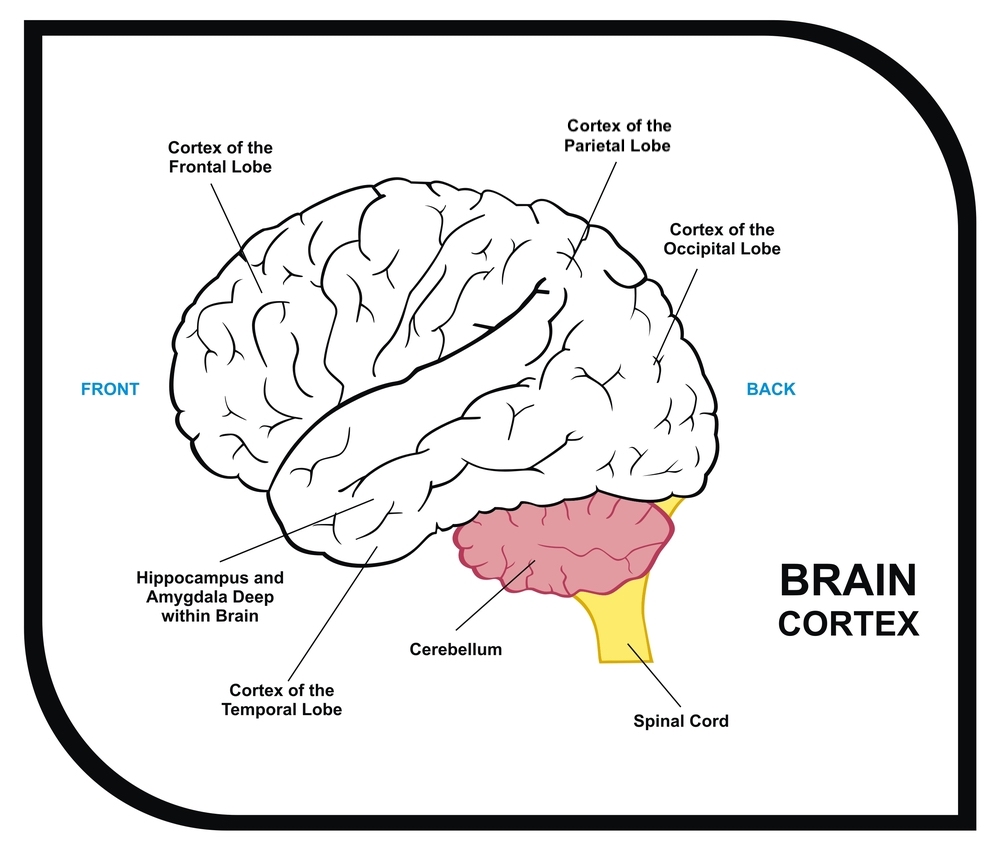
Younger patients can also experience an atypical form of Alzheimer’s disease. Up to 1 in 3 younger patients with Alzheimer’s disease have this unusual form compared to 1 in 20 older patients. The symptoms of Alzheimer’s vary depending on what areas of the brain are affected:
- If it affects parts of the brain located in the back of the head, it may cause problems with understanding visual information. For example, patients may struggle to read or judge distances. This is called posterior cortical atrophy.
- If it affects the sides of the brain (temporal lobe), symptoms include difficulties with speech, such as problems finding the right word or difficulty following a conversation. This is called logopenic aphasia.
- If it affects the frontal areas of the brain, it may cause memory problems and difficulties with planning and decision making. Patients may also behave in socially inappropriate ways. This is known as behavioral or dysexecutive Alzheimer’s disease.
Familial Alzheimer’s Disease
Familial Alzheimer’s disease is an extremely rare form of Alzheimer’s disease, accounting for fewer than 1 in 100 patients. It is caused by genetic mutations in three particular genes: PSEN1 (presenilin 1), PSEN2 (presenilin 2), and APP (amyloid precursor protein).
Having a parent or grandparent with young-onset Alzheimer’s suggests that at least one of these mutations runs in the family. This means there is a 50% risk of a parent passing on this form of dementia to their children. Symptoms typically start in the patient’s 30s or 40s. The earlier the symptoms develop, the more likely it is familial Alzheimer’s.
It is possible to do genetic testing for these mutations, but it’s important to consider the pros and cons of getting tested. On one hand, it may affect eligibility for medical and life insurance, but on the other hand, it will allow patients to plan for their family’s future.
Frontotemporal Dementia
Frontotemporal dementia involves damage to the lobes at the front and sides of the brain. This form of dementia is more common in younger patients than in older patients with dementia, and most cases are diagnosed in patients between the ages of 45 and 65.
About a third of patients with frontotemporal dementia have a family history of dementia. However, only about 10% of patients with this condition have familial frontotemporal dementia caused by a known gene mutation. The rest involve a variety of genes that can increase the risk of developing this type of dementia, but it’s not yet possible to test for these susceptibility genes.
Vascular Dementia
Vascular dementia develops due to problems in the blood supply to the brain. Symptoms vary from person to person but usually include a slower speed of thought, as well as difficulty solving problems and making decisions.
Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL) and cerebral amyloid angiopathy (CAA) are rare forms of vascular dementia that affect young patients. Symptoms, which include headaches, loss of mental abilities, and depression, usually start when patients are in their mid-30s. This form of dementia is caused by a genetic mutation and is usually inherited from a parent who has a 50% chance of passing on the mutated copy of the gene.
Late-Onset Forms of Childhood Neurodegenerative Disorders
Late-onset forms of some childhood neurodegenerative disorders can be mistaken with early-onset dementia in patients under age 35. The list of childhood neurodegenerative disorders includes mitochondrial disorders, lysosomal storage disorders, and leukodystrophies. A detailed family history is critical for diagnosis as many of these have hereditary features. Unfortunately, as with early-onset dementia, there are currently no treatments that can completely reverse these diseases once neuronal death has occurred.
Reversible Forms of Young-Onset Dementia
Young patients showing dementia symptoms may be suffering a reversible form of young-onset dementia. These conditions may include inflammatory and infectious diseases, metabolic disorders, and conditions triggered by excessive use of alcohol and drugs.
One example is alcohol-related dementia, which develops as a consequence of drinking excessive amounts of alcohol over several years. Patients diagnosed with this type of dementia tend to be in their 40s and 50s and represent about 10% of patients with early-onset dementia. Symptoms include difficulties with thinking, problem solving, attention, and controlling emotions. Patients can also experience changes in personality, difficulties learning new skills, and disorientation. This type of dementia is reversible. If patients stop drinking alcohol and receive treatment, there’s a good chance they will improve.
Further reading: What can make dementia worse
Treating Early-Onset Dementia

Although there are no treatments to cure dementia at the moment, there are several pharmacological and non-pharmacological approaches to slow down the progression of symptoms and increase the patient’s quality of life. An accurate diagnosis during the early stages of the disease is key to allowing patients to start their treatment as quickly as possible and reap the benefits for longer.
Treatment for early-onset dementia involves the same elements as for older patients. We’ll mention a few options here, but we’ve covered treatment options in more detail in another article looking at interventions to help dementia patients.
Pharmacological Approaches
There are a few FDA-approved prescription drugs to treat dementia. Unfortunately, these are not suitable for every patient and are associated with multiple side effects. Some patients may find it beneficial for a while, but we believe medication should not be considered the only way to address symptoms.
Current prescription drugs available include:
Aducanumab
This drug targets and removes beta-amyloid protein fragments found in the brain of patients with Alzheimer’s disease. The aim is to stop the cognitive and functional decline experienced by patients. Results show that the drug reduces amyloid accumulation, but that does not translate into significant cognitive benefits. In addition, patients experienced worrying side effects such as swelling and bleeding in the brain, headaches, dizziness, nausea, confusion, and vision changes. Aducanumab has been approved by the FDA for use in Alzheimer’s patients, but this decision has been heavily criticized by many health professionals. If you want to find out more, we’ve written in more detail about this drug and our reservations regarding its use in our article on how to help dementia patients.
Cholinesterase Inhibitors (Donepezil, Brand name: Aricept; Rivastigmine, Brand name: Exelon; Galantamine, Brand name: Razadyne)
These drugs affect the level of acetylcholine in the brain in patients with Alzheimer’s disease. This chemical plays a vital role in the brain by helping brain cells communicate with each other. Patients may see improvements in memory, thinking, language, judgment, and decision-making while taking this drug.
The use of these medications for young patients with other forms of dementia is still under investigation, although clinical trial results in frontotemporal dementia and CADASIL were disappointing.
Glutamate Regulators (Memantine, Brand name: Namenda)
These drugs help control the levels of glutamate in the brain. As dementia progresses, nerve cells start to release excessive amounts of glutamate, which block communication channels between different areas of the brain and cause cognitive decline. These drugs can improve memory, attention, reasoning, and language.
In addition to helping patients with Alzheimer’s disease, there’s some evidence that these drugs can also help patients with Lewy bodies dementia, vascular dementia, and mixed dementia. Unfortunately, clinical trials in young patients with frontotemporal dementia have failed to demonstrate any benefit.
Drugs to Treat Challenging Behavior
Many patients during the later stages of dementia develop emotional and psychological symptoms, including agitation, aggression, and hallucinations. For extreme or persistent cases, doctors can prescribe antipsychotic drugs such as risperidone or haloperidol. The Alzheimer’s Society recommends that these meds should be used at the lowest possible dose and only for short periods.
Non-pharmacological Interventions
There are also many therapies available to address dementia symptoms, from balance and depth-perception issues to cognitive difficulties and problems sleeping.
Physical Therapy (Physiotherapy)
Physiotherapists work closely with dementia patients to encourage physical exercise in order to maintain independence for as long as possible. Engaging in regular exercise can help both physical and cognitive skills in patients with early onset dementia. Regular sessions also improve the patient’s quality of life and promote social interactions.
Further reading:
Occupational Therapy
Occupational therapists work with dementia patients to help them live independently for as long as possible. This may include suggesting regular physical exercise to maintain fitness, encouraging patients to stay socially active, and developing brain games to promote cognitive skills.
For patients with early-onset dementia, one important way in which occupational therapists can help is by providing support to return to work after a diagnosis. Therapists can advise on whether to remain at the same job or seek alternative employment, suggest modifications to the work environment, and help patients rebuild their workplace skills.
Further reading: Occupational therapy for dementia patients
Cognitive Stimulation Therapy

Cognitive stimulation therapy (not to be confused with cognitive behavioral therapy) includes activities designed to help patients improve their memory, problem-solving skills, and language abilities. Patients can engage in a variety of activities and games, such as puzzles, crosswords, listening to music, or arts and crafts projects.
A study found that this type of therapy can help patients with early-onset dementia improve their cognitive skills, help with activities of daily living (ADLs), and reduce symptoms of anxiety and depression.
Further reading: Memory therapy for dementia patients
Talk Therapy (Psychotherapy)
Psychotherapy involves sessions with a counselor, a psychologist, or a psychiatrist. These interactions can be extremely helpful for patients with early-onset dementia who are struggling with an unexpected diagnosis. In addition, patients with early-onset dementia (especially those with frontotemporal dementia) are also more likely to develop depression or apathy, as well as behavior issues such as aggression and restlessness. All of these conditions may benefit from psychotherapy.
Speech and Language Therapy
Speech and language therapists help patients with communication and language issues, such as difficulty with attention and focus, speech problems, and difficulty reading. This type of therapy is particularly helpful for patients with frontotemporal dementia who are experiencing language problems such as speaking very slowly, struggling to say certain words, getting words in the wrong order, or using words incorrectly.
Other types of therapy
There are many other types of therapy that may be useful for patients with early-onset dementia. Many are focussed on keeping the patients engaged and socially active for as long as possible.
Some examples include:
- Reminiscence Therapy: During therapy, patients reminisce about past events. The aim is to stimulate mental activity and long-term memory. Therapists often use a variety of props, such as videos, music, pictures, and objects that hold a particular meaning for the patient. It’s aimed especially at patients with mild to moderate dementia, but even patients in the later stages of the disease can benefit from looking at old photos or listening to their favorite music.
- Art Therapy: Patients with dementia enjoy being involved in creative activities, such as sculpting, painting, drawing, or creating jewelry. These activities help ameliorate behavior issues and give patients a sense of accomplishment and purpose by providing an opportunity for nonverbal expression. Curiously, younger patients with frontotemporal dementia show high levels of creativity, even when other cognitive skills start to deteriorate. They may greatly enjoy these sessions.
- Massage and Aromatherapy: These sessions can have a calming effect on patients suffering with dementia. Therapists can use essential oils to relieve stress and promote well being. For example, lavender, chamomile, and lemongrass can be used to promote relaxation.
- Music Therapy: Music therapy during all stages of dementia may improve behavior problems, lower anxiety, and control agitation. Patients can play a musical instrument, sing, or attend musical concerts, for example. As symptoms worsen, patients can still enjoy listening to familiar songs and thinking about happy memories from the past.
- Pet Therapy (Animal-Assisted Therapy): This therapy can be beneficial for patients who love pets. Petting a cat or going for a walk with a dog reduces behavioral symptoms, such as agitation and aggression, and improves the patient’s mood.
- Sensory Stimulation Therapy (Sensory Integration Therapy): This therapy helps patients remember positive emotions and memories by triggering one of the five senses: hearing, sight, smell, taste, or touch. The aim is to make patients feel relaxed, as well as to improve their self-esteem and well-being.
- Bright Light Therapy: Sleep problems and disruptive behavior at night are common in dementia patients. Bright light therapy can be used to treat these sleep disturbances. Patients need to sit in front of a light box that provides about 30 times more light than the average light for a set amount of time. The aim is to reset the patient’s internal clock and help them get a good night’s sleep.
Combination of Physical and Cognitive Therapies
At Neural Effects, we base our treatment protocols on studies showing that a combination of exercise and therapy is much more effective than each therapy in isolation. Physical exercise triggers a phenomenon in the brain called post-exercise cognitive boost (PECB). During PECB, the brain releases an important chemical called brain-derived neurotrophic factor (BDNF), which makes the brain more receptive to therapy. This approach to treatment is not available from every provider.
Before treatment starts, patients undergo a neuropsychological exam (also called a neurocognitive evaluation) to find out how dementia has affected their cognitive skills. The results allow our therapists to tailor treatment to the patient’s needs and establish a baseline to reference over time. Our team will also assess physical abilities, such as reflexes, eye movements, balance, and posture. Finally, we evaluate patients for signs of anxiety, depression, or stress.
After all these exams, patients and their loved ones meet with a member of our team to discuss possible treatments. Our treatment program involves cardiovascular exercise followed by therapies such as cognitive therapy, neuromuscular therapy, and occupational therapy. This multidisciplinary approach is more effective than therapies which are administered one-by-one with minimal communication between therapists.
Patients are encouraged to bring a family member to the sessions so that they can learn the exercises and help them at home. In addition, at the end of each session, patients receive a series of exercises to do at home. Completing these exercises is a good way to improve the overall effect of therapy.
Neural Effects uses the latest evidence-based techniques to diagnose and help dementia patients. We are located in Provo, Utah and serve anyone in Salt Lake City or the Utah Valley area. We are in network for most types of medical insurance. Schedule your evaluation today.
Strategies for Living With Early-Onset Dementia

Younger patients with dementia experience a range of challenges which are often very different compared to those older patients experience. Dementia is harder for younger patients because it comes at a time in their lives when it is least expected and can affect both work and family life. To further complicate matters, limited support services specifically designed for patients with younger-onset dementia often causes patients and families to feel isolated or overwhelmed.
Here, we look at some problems that can arise for patients with early-onset dementia and suggest possible solutions:
Relationship with a partner
Some couples may find that their relationship changes after a dementia diagnosis. When one partner receives a diagnosis of dementia, the couple needs to assess how their relationship works and what may need to change. Unfortunately, as symptoms progress, both partners will have to adapt more.
The best policy is always to communicate with each other and to make time for leisure activities that both partners can enjoy together. Counseling can be helpful in this time of transition.
Children
Younger patients with dementia are more likely to have children still living at home. Dementia can have a big impact on them, especially in very young children who may not understand why their mom or dad is changing. It can be hard to explain, but it’s important to be honest with children and listen to their concerns.
In addition, if the patient has a genetic form of dementia, it can have immense repercussions for the children. It’s not uncommon for the patient to feel guilty about putting their children at risk. In turn, children may be angry or unsure about how to deal with the situation and whether they should be genetically tested. It can be helpful to have access to trained support and counseling for the entire family to deal with these issues.
Employment
Many younger patients start to notice symptoms because they struggle with something at work. They may forget important meetings or find it difficult to follow a conversation.
Some patients opt to continue working for as long as possible, while others prefer to stop. Making this decision can be difficult and can have significant implications for the rest of the family, especially in terms of income. Where possible, staying in some form of employment (even if it’s only part-time or voluntary) can be very beneficial for patients with dementia.
Finances
People with early-onset Alzheimer’s often have to stop working or find a part-time job, which means a loss of income. Finances get even worse if partners also need to become full-time caregivers. This can cause stress and worry, especially if patients have a range of financial commitments like a mortgage or bank loans.
Financial advisers and lawyers may be able to help families plan for future needs. This may include, for example, exploring what benefits are available or how to arrange an early retirement.
Driving
When dementia patients are no longer able to think clearly and make quick decisions, they should stop driving, as they may not be able to deal with any unexpected situations on the road. For family members and carers, signs that the patient may be struggling to drive include new dents and scratches in the car, taking a long time to drive somewhere local, or getting traffic tickets for dangerous driving.
State laws vary regarding when a patient with dementia should stop driving. It’s important to check with your state’s Department of Motor Vehicles for more information.
Planning for the future
Patients may feel better if they have a plan for the future to manage their financial, legal, and medical affairs. This may include:
- Organizing living arrangements for the future.
- Deciding who can have access to financial records and bank accounts.
- Talking to a financial adviser.
- Sorting out health and income insurance.
- Writing or updating a will.
- Nominating a trusted person to manage any affairs in the future.
Ways to Delay Progression of Dementia Symptoms at Home

The following activities can help patients maintain independence for as long as possible and slow down neurological decline:
Staying active is crucial to the wellbeing of patients with early-onset dementia and in delaying progression of symptoms. Ideally, physical activity should include a combination of cardio exercise, strength training, balance, and coordination exercises. Patients do not have to engage in extreme amounts of exercise. At least 30 minutes every day, five days a week is ideal. Good activities for dementia patients include walking, swimming, yoga, and gardening.
Especially if the patient had to give up work because of their diagnosis, finding new activities and hobbies can help them keep their brain engaged and active. Activities to help patients recall information, think quickly, solve problems, or make decisions can protect cognitive skills. For example, patients can learn something new, read at a slightly harder level than is normal for them, play a musical instrument, or engage in arts and crafts.
Younger patients with dementia need to stay socially active and continue doing their normal activities as much as possible. Some patients stop going out and prefer to stay at home. This not only accelerates progression of symptoms, but can also make friends unsure how to act around them or even question their diagnosis, which can cause further social isolation. Social interaction can take many forms, such as volunteering at a local charity, joining a book club or a support group, going out regularly with friends, or simply phoning a family member.
Finally, dementia patients should follow a healthy and balanced diet to reduce inflammation and protect the brain. The MIND diet — which combines a traditional Mediterranean diet and the DASH diet designed to lower blood pressure — can slow down brain aging equivalent to 7.5 years. This diet focuses on vegetables, fruits, nuts, whole grains, low-fat dairy products, and lean protein foods, while avoiding salty, sugary, and fatty processed foods.
Neural Effects uses the latest evidence-based techniques to diagnose and help dementia patients. We are located in Provo, Utah and serve anyone in Salt Lake City or the Utah Valley area. We are in network for most types of medical insurance. Schedule your evaluation today.
